Jennifer Robyn Bernard, widely recognized for her portrayal of Terry Brock on General Hospital, has sadly passed away. A well-known figure to soap opera enthusiasts during the 1980s, Bernard appeared in 145 episodes of the iconic series from 1984 to 1990, leaving a lasting impact on viewers who remember her compelling performances.
Authorities confirmed that Bernard’s body was discovered earlier this week in San Jacinto, California. Law enforcement responded to a report concerning an unattended death on Tuesday, and her identity was verified through fingerprint records. An autopsy is planned by the Riverside County Coroner’s Office, but the official cause of death remains undisclosed.
Beyond her significant role on General Hospital, Bernard also took on the role of a psychologist in the 2002 film Voices from the High School. Although she largely stepped away from acting following her daytime TV career, she remained a cherished figure among fans and those who worked alongside her.
Her passing comes shortly after the General Hospital community was already grieving the loss of another beloved star, Jackie Zeman, known for her role as Bobbie Spencer
Jugular Venous Distension: A Clinically Important Sign
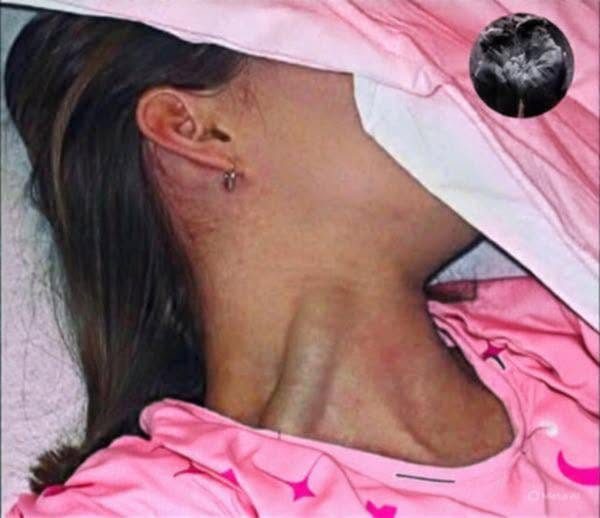
Jugular venous distension (JVD) is a physical finding that can be seen at the bedside without any machines or lab tests. It refers to the visible bulging of the jugular veins in the neck, caused by an increase in central venous pressure (CVP). This simple but important sign often points to significant cardiovascular problems and should never be ignored.
Why Are the Jugular Veins So Important?
The jugular veins run along the sides of the neck and drain blood from the head and neck back into the heart. They connect directly to the superior vena cava and then to the right atrium. Because of this direct connection, any rise in right atrial pressure is quickly reflected as distension of the jugular veins.
In other words: the jugular veins act like a natural “barometer” of right-sided heart function.
Common Causes of Jugular Venous Distension
Several medical conditions can lead to jugular venous distension. Among the most frequent and important are:
-
Right-Sided Heart Failure
When the right ventricle cannot effectively pump blood into the lungs, blood backs up into the venous system. This causes swelling of the legs (peripheral edema), fluid buildup in the abdomen (ascites), liver enlargement, and distended jugular veins. -
Superior Vena Cava Obstruction (SVC Syndrome)
A tumor, blood clot, or other obstruction in the superior vena cava prevents blood from draining from the head and neck. Patients often have facial swelling, bluish discoloration (cyanosis), and visible, engorged neck veins. -
Cardiac Tamponade
This is a medical emergency in which fluid accumulates around the heart in the pericardial sac. The pressure prevents the heart chambers from filling properly. Venous blood cannot enter the right atrium, and jugular venous distension becomes strikingly visible. -
Pulmonary Hypertension
Chronic high pressure in the pulmonary arteries strains the right ventricle, eventually leading to right heart failure and venous congestion. -
Tricuspid Valve Disease
Incompetence of the tricuspid valve allows blood to leak backward into the right atrium during ventricular contraction, increasing venous pressure and distending the jugular veins.
Beck’s Triad and Cardiac Tamponade
One of the most dramatic associations of jugular venous distension is with Beck’s Triad, the classic clinical presentation of cardiac tamponade. The triad includes:
-
Low blood pressure (hypotension) – because the heart cannot fill and pump effectively.
-
Jugular venous distension – due to impaired venous return.
-
Muffled or distant heart sounds – as fluid around the heart dampens the sound.
The simultaneous presence of these three signs indicates a life-threatening condition that requires immediate intervention, typically pericardiocentesis (removing fluid with a needle).
Diagnostic Value
For physicians, observing the jugular veins is one of the simplest and most informative bedside tests. With the patient reclining at about a 45-degree angle, the height of the jugular venous column can be estimated, giving an indirect measure of central venous pressure.
This physical finding is often complemented by further investigations such as echocardiography, chest imaging, or ultrasound of the neck veins to determine the underlying cause.
Treatment and Prognosis
The management of jugular venous distension depends entirely on the underlying condition:
-
Right heart failure: diuretics, ACE inhibitors, beta blockers, and lifestyle modification.
-
Cardiac tamponade: emergency pericardiocentesis or surgery.
-
SVC syndrome: treatment of the underlying cause, such as anticoagulation, stenting, or cancer therapy.
-
Pulmonary hypertension: medications to reduce pulmonary vascular resistance and supportive care.
-
Valve disease: surgical repair or replacement may be required.
The prognosis varies widely. While acute tamponade is life-threatening, chronic right heart failure can be controlled with proper therapy.
Conclusion
Jugular venous distension may seem like a small physical sign, but it is one of the most revealing indicators of serious heart and circulatory problems. Because the jugular veins reflect right atrial pressure, their engorgement points directly to underlying pathology such as heart failure, SVC obstruction, pulmonary hypertension, tricuspid valve disease, or cardiac tamponade.
In particular, its role as part of Beck’s Triad makes it a crucial red flag for cardiac tamponade — a condition that can be fatal without immediate treatment.
For clinicians, the simple act of looking at the neck veins provides invaluable information. For patients, noticing unusual neck vein bulging should prompt urgent medical evaluation.